First demonstration of universal cancer vaccine
New data shows 27% improved survival for malignant mesothelioma patients in the NIPU trial.
Positive results from the NIPU trial announced last night show the combination of a universal cancer vaccine and checkpoint inhibitors in patients with malignant mesothelioma reduces the risk of death by 27%.
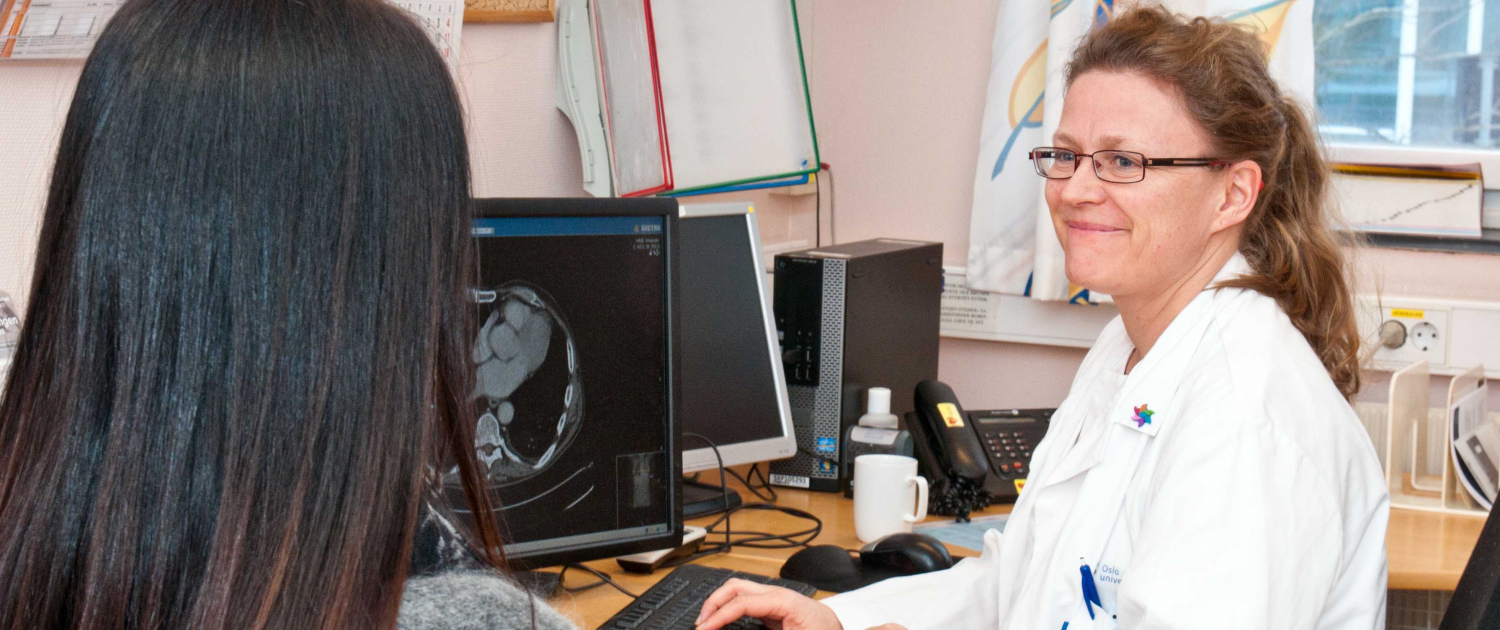
“For patients with malignant mesothelioma, few treatment options are available after first-line chemotherapy. The NIPU study showed that patients receiving UV1 vaccination as add-on to nivolumab and ipilimumab experienced an increased objective response rate and a clinically meaningful prolonged survival. These encouraging results provide a foundation for advancing further clinical development with UV1 vaccination in mesothelioma patients,” said Principal Investigator of the NIPU clinical trial, Professor Åslaug Helland, MD Ph.D.

Åslaug Helland, Principal Investigator of the NIPU clinical trial. Photo: Per Marius Didriksen, Oslo University Hospital
The ‘gold standard’
This is the first demonstration of the efficacy and therapeutic impact of a universal cancer vaccine in a Phase II trial. The universal cancer vaccine is the lead product of the Norwegian biotech company Ultimovacs, which is developing novel immunotherapies against cancer. The vaccine is currently being tested in five Phase II trials on different cancer indications.
“We are thrilled to announce the highly advantageous results from the first randomized UV1 Phase II trial, marking a major milestone for Ultimovacs. Overall survival is the ‘gold standard’ in cancer treatment. We believe these data support further development in mesothelioma, and we are looking forward to discussing the results with the regulatory authorities,” said Carlos de Sousa, CEO of Ultimovacs.

Carlos de Sousa, CEO of Ultimovacs. Photo: Ultimovacs
Since malignant mesothelioma is a hard-to-treat cancer, the positive results from the NIPU trial give cause for optimism in the ongoing Ultimovacs’ trials for other cancer indications too, including malignant melanoma, head and neck cancer, ovarian cancer, and non-small cell lung cancer.
In October 2023, the FDA ranted Orphan Drug Designation for UV1 in the treatment of mesothelioma, but there is still a way to go before the drug reaches the market. The treatment has to be assessed in a Phase III trial and undergo regulatory approval before becoming widely available.
Improved survival and response rate
Oslo University Hospital leads the NIPU study with support from Ultimovacs and Bristol-Myers Squibb. It includes 118 patients from Norway, Sweden, Denmark, Spain and Australia. The patients are in second-line treatment, which means they already received chemotherapy without beneficial results and have no other treatment options.
The patients were divided into two randomized groups: 59 patients received the universal cancer vaccine in combination with checkpoint inhibitors, and the other group received only checkpoint inhibitors. Results show that patients who received the universal cancer vaccine had a prolonged survival rate and a significantly better objective response rate. This means the patients lived longer and more patients’ tumours shrunk than in the control arm. In addition, the treatment showed no added side effects.
“We want to extend our gratitude to the patients and their families, as well as the dedicated investigators and all our supporters whose invaluable contributions made this study possible,” Helland commented.
For more information, please read the press release from Ultimovacs or follow the company’s webcast on Mon, Oct 23 2023 at 14:30 (CET).
The post First demonstration of universal cancer vaccine first appeared on Oslo Cancer Cluster.




 Pixabay
Pixabay

